Category Archives: Uncategorized
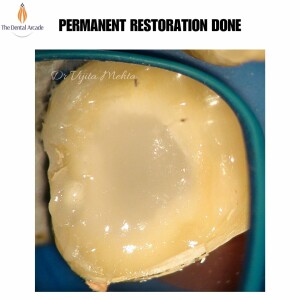
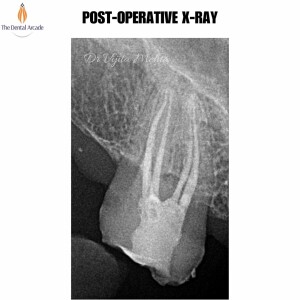
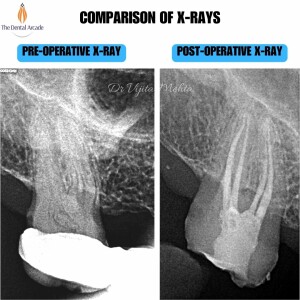
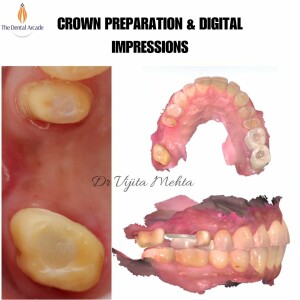
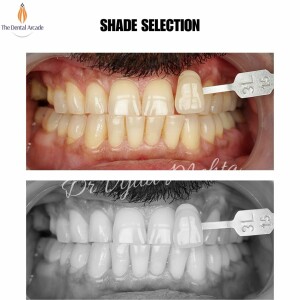
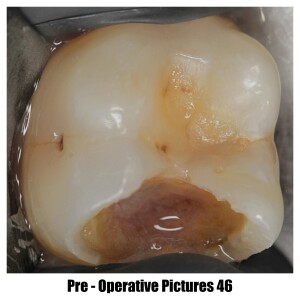
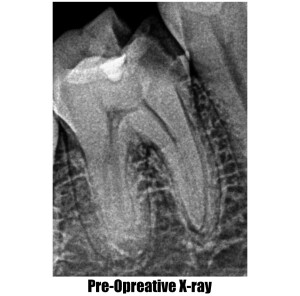
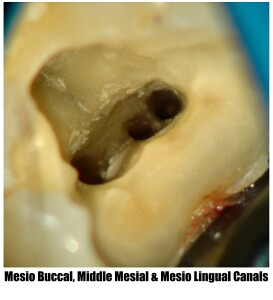
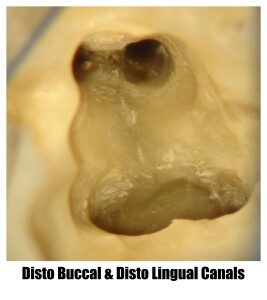
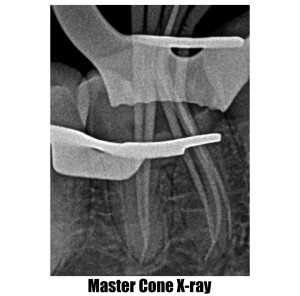
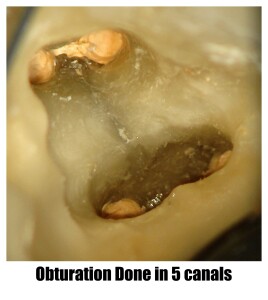
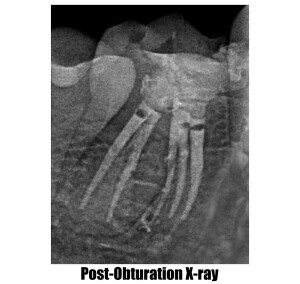
Root Canal Treatment (Part-2)
Women Empowerment Award
“Winning an award is a moment of triumph, where one’s efforts are celebrated and acknowledged by peers and experts in the field. Awards serve as a symbol of excellence and often motivate individuals to continue striving for greatness in their endeavors.”
Reveling in Dr. Vijita Mehta’s extraordinary accomplishment as one of the esteemed 15 recipients of the Women Empowerment Award in Chandigarh stands as a resounding testament to her unwavering commitment and invaluable contributions towards society.
This event unfolded in the splendid setting of the DLF City Centre IT Park in Chandigarh, coinciding with the premiere of the Punjabi cinematic gem, “Chidiya Da Chamba.” Graced by the presence of the movie’s illustrious cast, it was an evening dedicated to celebrating the indomitable spirit of womanhood through the bestowal of awards and well-deserved recognitions.
Root canal treatment
Synergetic session on goal of developed India by Dr Vijita mehta
📢 Exciting Event Announcement! 🇮🇳🗣️
Thrilled to have been a part of the inspiring Yuva Samvad-India @ 2047 program, organized by the Nehru Yuva Kendra Chandigarh and Yuva Stambh Sanstha, under the guidance of District Youth Officer, Ms. Sanjana Vats.
The event took place at the prestigious Government Model Senior Secondary School Sector 26, Timber Market Chandigarh.
As one of the speakers, Dr. Vijita Mehta along with Mrs. Manjula Salaria, Mrs. Kamakshi Malik, and Mrs. Kiran Bala, had an engaging discussion with the students about the Panch-Pran of the Amritkal of freedom. The focus was on fostering national unity and solidarity, instilling a sense of duty among citizens, envisioning a developed India, taking immense pride in India’s rich heritage, and eradicating any remnants of slavery or colonial mindset.
The enthusiasm displayed by the students was remarkable! They actively participated, sharing their thoughts, and learning about their crucial roles as responsible citizens and their deep-rooted pride in our nation’s heritage. We were also thrilled to hear about the remarkable achievements and contributions of Nehru Yuva Kendra, as shared by the Accounts and Program Assistant, Ms. Preetika.
At the conclusion of the event, all the guests were honored, and together, they took a pledge to make the Amrit Mahotsav of Independence a resounding success. 🙌
Yuva Stambh President Upendra Kumar provided great support in making the programme successful.
Bulimia
The dental changes seen in many of us with bulimia are often recognizable. Frequent vomiting may cause your salivary glands to swell and therefore the tissues of your mouth and tongue to become dry, red and sore. People with bulimia may have chronic pharyngitis and little hemorrhages under the skin of the palate.
Frequent vomiting can erode your enamel , especially on the tongue side of the upper front teeth. This sharply increases the danger for decay in these areas and may make these teeth sensitive to temperature. Severe erosion can cause changes in your bite, or the way your upper and lower teeth close . Your back teeth are often reduced in size and a few teeth can even be lost eventually. Tooth erosion can take about three years to become obvious, but not all bulimics experience it.
Many people with bulimia could also be malnourished, which may cause anemia, poor healing and increase the danger of periodontitis .
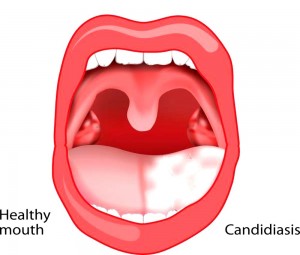
Thrush
Thrush (also called Candidiasis or moniliasis) is a fungal infection that occurs when the yeast Candida albicans reproduce in large numbers. It is common among denture wearers. Most often it occurs in people with weak immune systems—the very young, elderly or those debilitated
by disease, such as diabetes or leukemia. In addition, people with dry mouth syndrome are susceptible to candidiasis. Candida may also flourish after antibiotic treatment, which can decrease normal bacteria in the mouth.
Controlling candidiasis means focusing on preventing or controlling the condition that causes the outbreak.
Good oral hygiene is essential. Clean your dentures to remove Candida and remove them at bedtime. If the cause is dry mouth saliva substitutes and prescription medications may be helpful when the underlying cause of dry mouth is incurable or unavoidable.
What Are the Symptoms?
White, slightly raised areas in your mouth are common signs of thrush. They’re usually found on your tongue or inner cheeks. They can also appear on the roof of your mouth, gums, tonsils, or the back of your throat. These areas may look like cottage cheese. They can be painful and may bleed slightly when you scrape them or brush your teeth.
In very bad cases, they can spread into your esophagus and cause:
• Pain when you swallow or difficulty swallowing
• A feeling that food is stuck in your throat or in the middle of your chest
• Fever, if the infection spreads beyond the esophagus
The fungus that causes thrush can spread to other parts of the body, like the lungs, liver, and skin. This happens more often in people with cancer, HIV, or other conditions that weaken the immune system.
How Will I Know if I Have It?
Your dentist or doctor can probably tell by taking a look inside your mouth. Your doctor might also send a tiny sample of the spot to a lab just to make sure.
If the fungus that causes thrush spreads into your esophagus, you may have to have other tests,
like:
• A throat culture (a swab of the back of your throat)
• An endoscopy of your esophagus, stomach, and small intestine
• X-rays of your esophagus
What’s the Treatment?
Thrush is easy to treat in healthy children and adults. But the symptoms may be worse and
harder to treat in people with weak immune systems.
Your doctor will probably prescribe antifungal medications that you’ll have to take for 10 to 14
days. These come in tablets, lozenges, or liquids, and are generally easy to take.
Since the infection can be a symptom of other medical problems, your doctor may also want to
run other tests to rule these out.
How Can I Prevent Thrush?
- Practice good oral hygiene. Brush your teeth at least twice a day and floss at least once a day.
- Get regular dental checkups. Especially if you have diabetes or wear dentures.
- Even if you’re healthy and don’t have dental issues, you should get your teeth cleaned by your dentist every 6
months.
DENTAL CAMP
THE DENTAL ARCADE organized a free dental check up and awareness camp at S D college sector 32 chandigarh . Over 50 employees and their families were examined and provided with required dentifrices free of cost.
Apart from check-up, the staff were made aware about dental health and hygiene by the team of experts doctors.
Dr Vijita explained that most of the dental diseases can be prevented by simple practice of brushing twice daily with soft brush and regular dental check-up.
She also told that the modern eating habits are one of the biggest reasons for dental problems.
If we regularly visit our dentist and follow good eating habits we can avoid oral problems.
The camp was initiated with dental awareness talk, educating people about common dental ailments, especially stressing on tooth decay and gum diseases and measures to prevent from them.
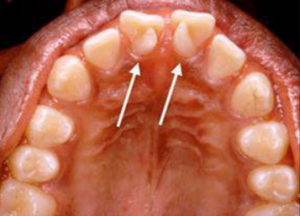
Talon Cusp
Meaning of Talon Cusp:-
Talon cusp is a rare dental anomaly. Generally a person with this develops “cusp-like” projection
Located on the inside surface of the upper affected tooth. Talon cusp is an extra cusp on an anterior tooth. Although talon cusp may not appear serious.
Cause of talon cusp:-
The cause of talon cusp is unknown. The anomaly can occur due to genetic and environmental factors but the onset can be spontaneous. Prevention is difficult because the occurrence happens during the development of teeth.
Treatments of Talon cusp:-
Treatment is only required if the occlusion or bite of the person is compromised and causing other dental problems.
- Multiple long-term clinical problems can arise such as occlusal interferences, aesthetic disturbances, loss of pulp vitality, and irritation of tongue during mastication and speech, caries and displacement of the affected tooth.
- Most people with talon cusp will live their normal lives unless the case is severe and causes a cascade of other dental issues that lead to additional health problems.
Small talon cusps that produce no symptoms or complication for a person can remain untreated. However large talon cusps should not.
Some common treatments include:
- Fissure sealing
- Composite resin restoration
- Reduction of cusp
- Pulpotomy
- Root canal (endodontic treatment)
- Extraction
Sometimes it can cause mild irritation to soft tissues around the teeth and the tongue, and if large enough, may pose an aesthetic problem. Talon cusps that are too large are filed down with a motorized file, and then endodontic therapy is administered.
- In order to prevent any future dental complications, when large talon cusp is present due to an early diagnosis it would be best to see a dentist regularly every six months for routine dental checkups, remain under observation, brush and floss properly and undergo regular topical applications of fluoride gel to prevent caries and to promote enamel strength.
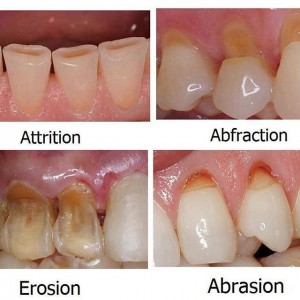
DIFFERENCE BETWEEN ABFRACTION, ABRASION, EROSION AND ATTRITION
DIFFERENCE BETWEEN ABFRACTION, ABRASION, EROSION AND ATTRITION
Abfraction, abrasion, erosion and attrition all involve some tooth damage, but at different locations on the tooth. While they have varying causes, they can interact and create a bigger problem. It’s possible to have abfraction, abrasion, erosion and attrition at the same time.
Abfraction
Abfraction is a wedge-shaped flaw on the tooth at the point it meets the gumline.
It’s caused by friction and pressure on the tooth and gums, which causes the neck of the tooth to start breaking off.
Abrasion
Abrasion is likely to be found on the teeth closest to your cheeks, also known as the buccal side. Unlike the V-shaped appearance of abfraction, the damage caused by abrasion is flat.
Abrasion is caused by friction from foreign objects, such as pencils, fingernails, or mouth piercings. Using a hard toothbrush, abrasive tooth products, and improper brushing technique can also lead to abrasion.
Erosion
Erosion is the general wearing away of tooth enamel. Teeth may have a more rounded appearance, with hint of transparency or discoloration. As erosion progresses, you can start to see dents and chips in the teeth.
Unlike abfraction and abrasion, erosion is more of a chemical process, happening on the surface and subsurface of the teeth. It’s caused by high acid levels in the saliva. This may be due to acidic foods or drinks, dry mouth, or health conditions that cause frequent vomiting.
Attrition
Dental attrition is a type of tooth wear caused by tooth-to-tooth contact, resulting in loss of tooth tissue, usually starting at the incisal or occlusal surfaces. Tooth wear is a physiological process and is commonly seen as a normal part of aging.